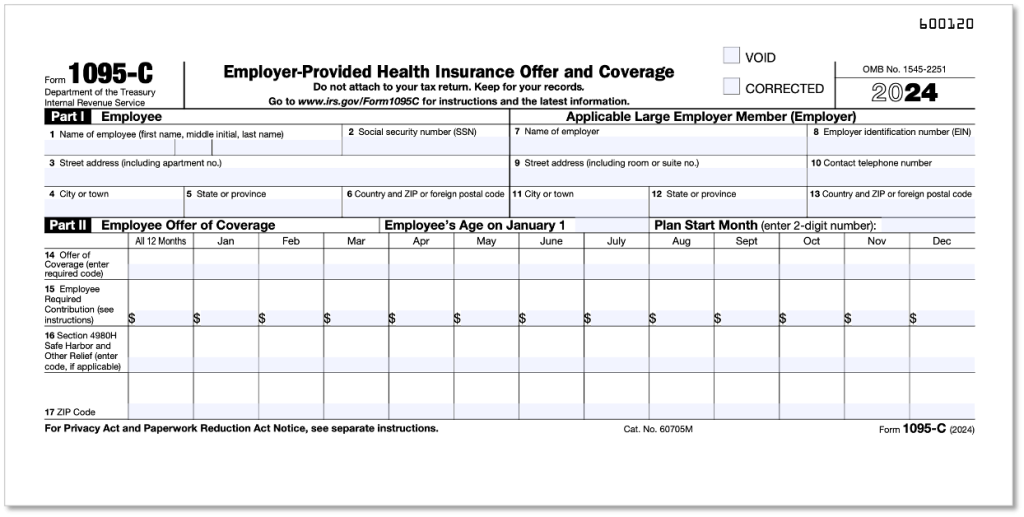
AI & RegTech for Employee Benefits [Part 1/3]
The AI revolution is fueling exciting and far-reaching business transformation — but also a good deal of hype, misunderstanding and even risk. Unlike other tehnology revolutions, many of the most avid early adopters of AI are the least expert. This can lead to organizations into misapplications, missed opportunities or, far worse, costly pitfalls and even unsafe […]
AI & RegTech for Employee Benefits [Part 1/3] Read More »